Melanoma
While melanoma is less common than other forms of skin cancer, it is the deadliest and is responsible for approximately 75% of all skin cancer deaths. Approximately 160,000 new melanoma cases are diagnosed in the U.S. each year. Excessive ultraviolet light (UV) exposure contributes greatly to one’s risk of developing melanoma.
Regular skin checks by a dermatologist are crucial in detecting Melanoma, a potentially life-threatening form of skin cancer. Dermatologists possess the expertise to identify suspicious moles, lesions, or changes in the skin that might indicate Melanoma. Equally important are self-exams, where individuals monitor their skin for any alterations in moles' shape, size, color, or the appearance of new spots.
By combining professional evaluations with self-examinations, early detection becomes more likely. Timely intervention significantly improves the chances of successful treatment and better outcomes for Melanoma, underscoring the importance of regular checks by both dermatologists and self-exams for everyone's overall skin health.
Your skin health is our top commitment at Brentwood Dermatology. Our expert providers are ready to take care of you and your loved ones throughout the entirety of their skin wellness journey.
Examples of Melanoma
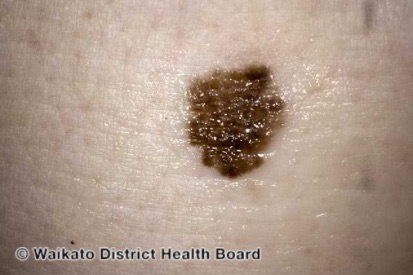
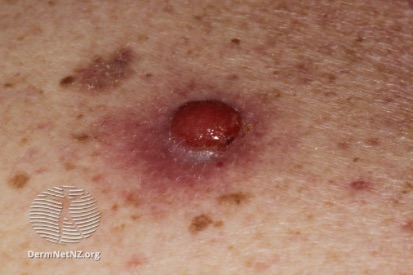
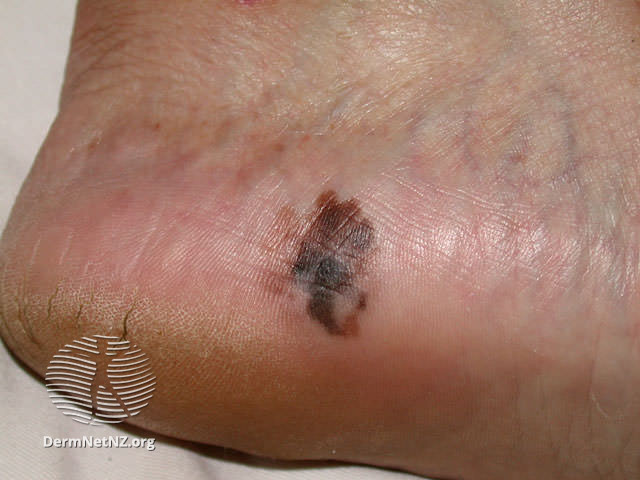
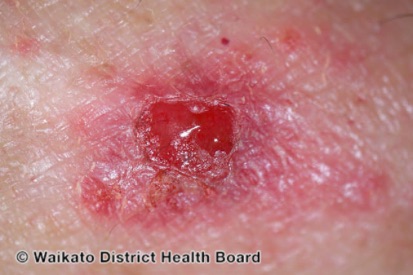
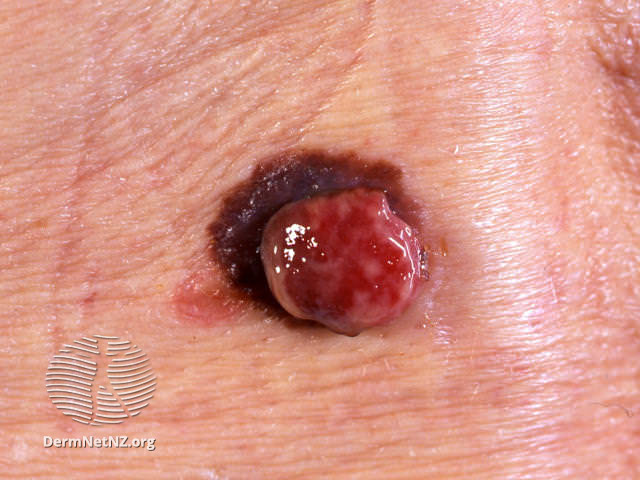
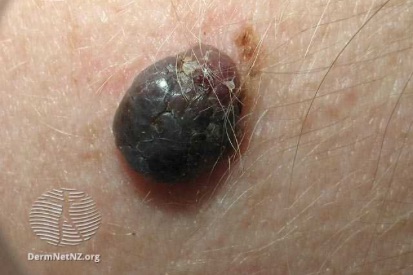
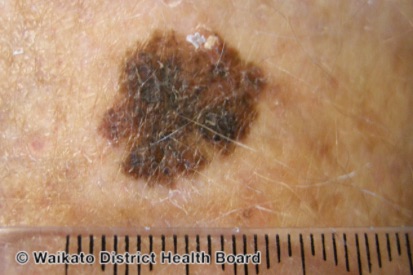
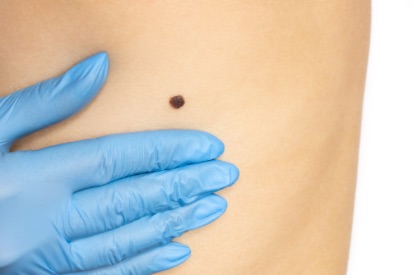
Symptoms of Melanoma
- Melanoma most often presents itself with the change of an existing mole, including change of symmetry, color, or shape.
- Irregular mole borders – scalloped, wavy, or notched.
- Diameter - anything new growing in size.
- Moles that itch, ooze or bleed.
- Melanoma can appear on normal skin tissue and does not always start as a mole.
What Causes Melanoma?
- Melanoma is primarily caused by the uncontrolled growth of pigment-producing cells (melanocytes) in the skin.
- Melanoma is often triggered by exposure to ultraviolet (UV) radiation from sunlight or tanning beds.
- Genetic factors and a history of severe sunburns also contribute to the development of melanoma.
How to Prevent Melanoma
Melanoma FAQs
The primary cause of melanoma is exposure to ultraviolet (UV) radiation, either from sunlight or tanning beds. Other risk factors include having fair skin, a history of sunburns, numerous moles, a family history of melanoma, and a weakened immune system.
Diagnosis involves a biopsy, where a sample of the suspicious area is removed and examined under a microscope. Dermatologists may use the ABCDE rule (Asymmetry, Border irregularity, Color variations, Diameter larger than 6mm, Evolution or change) to assess whether a mole may be melanoma.
Melanoma is staged from 0 to IV, with stage 0 being melanoma in situ (confined to the top layer of skin) and stage IV indicating the cancer has spread to other organs. Staging helps determine the extent of the disease and guides treatment decisions.
Treatment options for melanoma depend on the stage of the cancer and may include surgical excision, lymph node removal, immunotherapy, targeted therapy, radiation therapy, or chemotherapy. The choice of treatment is individualized based on factors such as the patient's overall health and the characteristics of the melanoma.
A skin check performed by a dermatologist involves a thorough examination of the skin to identify any abnormalities, including moles, lesions, or other signs of skin conditions or skin cancer. This examination may be part of a routine check-up or may be prompted by specific concerns. The dermatologist assesses the size, shape, color, and texture of moles, and may perform additional tests or biopsies if necessary for further evaluation. Regular skin checks are essential for early detection and management of skin issues, and, skin cancer.
You should apply sunscreen every day, regardless of weather. Even on cloudy days and during the winter, UV rays can still penetrate the clouds and cause skin damage. Sunscreen needs time to be absorbed into the skin. Apply it at least 15-30 minutes before going outdoors and reapply every two hours.
From our QualDerm Family of Brands: Melanoma Treatment Options
Melanoma Treatment Options
We will confirm melanoma through a biopsy and pathological examination and then treat appropriately.
Treatment options for melanoma provided by a dermatologist may include surgical procedures to remove the cancerous tissue, such as excision or Mohs surgery. Additionally, your dermatologist may recommend therapies like immunotherapy, targeted therapy, or chemotherapy, depending on the stage and characteristics of the melanoma. Close monitoring, regular skin checks, and collaboration with other specialists ensure effective treatment and reduce the risk of recurrence.
If you notice unusual growths on your skin as mentioned above, we highly recommend scheduling an appointment with one of our providers. Annual skin checks are essential for early detection.
Early detection and treatment are crucial elements of comprehensive skin cancer care.
Featured Products for Sun Protection

Colorescience Sunforgettable Total Protection Body Shield Bronze SPF 50
Enjoy a perfect, natural sun-kissed glow all year long without the damage! This powerful protector features a beautiful bronze tint with our exclusive EnviroScreen® Technology to provide all-mineral protection from environmental aggressors such as UVA/UVB, pollution, blue light, and infrared radiation. Patented ingredients and a hydrating, antioxidant-rich mineral formula nourish and protect skin against free radicals that contribute to skin damage. Total protection in an elegant texture that blends easily with a weightless finish. Net Wt. 4 fl. oz. / 120 mL

ZO® Gel Sunscreen Broad-Spectrum SPF 50
A clear and unscented gel sunscreen with a complexion-smoothing finish for all skin tones. Exclusive antioxidant + plant stem cell complexes minimize the aging effects of environmental aggressors. Water and sweat resistant up to 40 minutes. Fragrance-free. 45 g / 1.6 Oz.
